 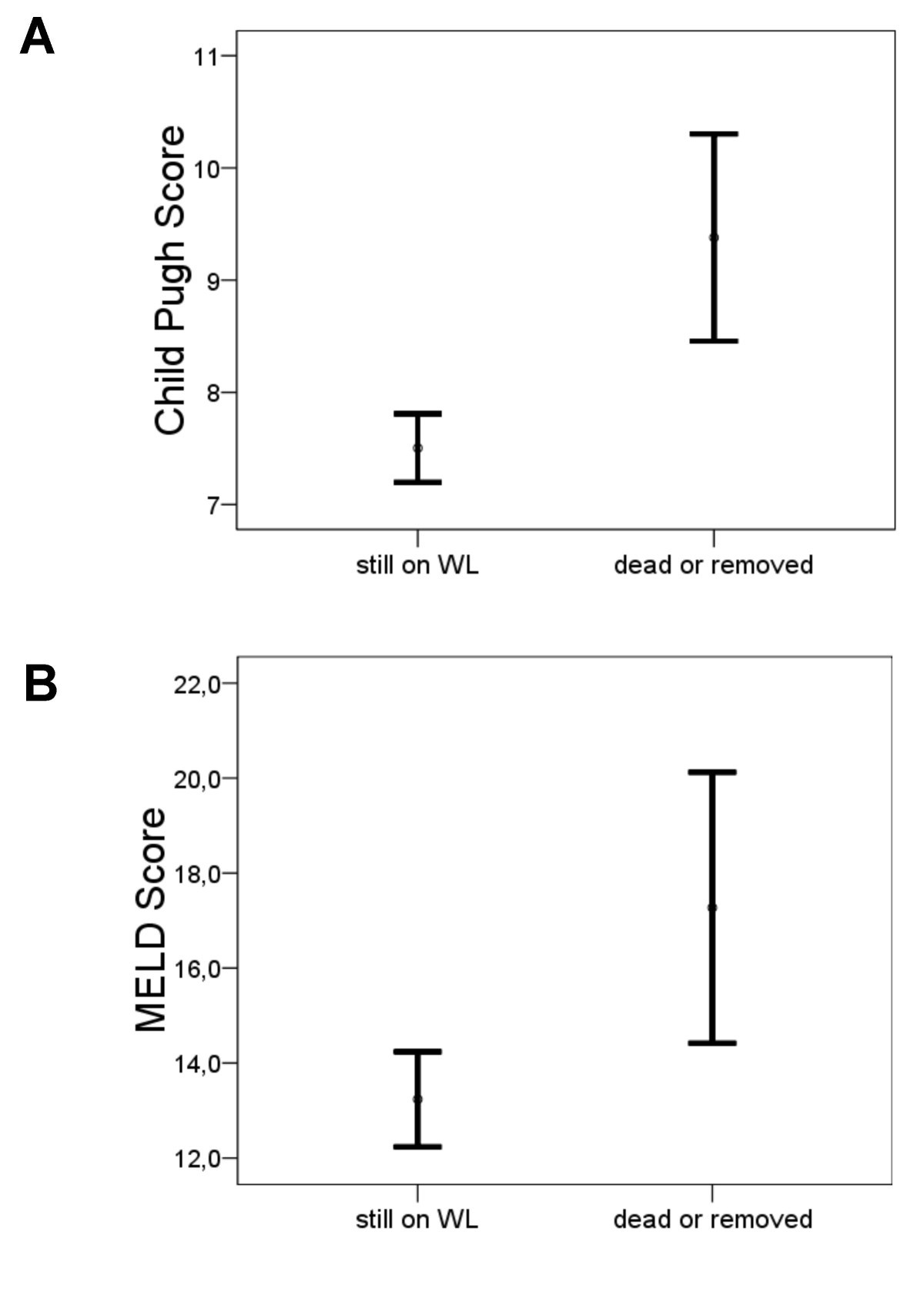
However, the MELD score has been criticized for several different reasons. This MELD score was found to be superior to the CTP score in predicting 3-months mortality and therefore the MELD score was implemented in 2002 in the United States for the prioritization of LTx recipients. A modification of this score was developed to predict mortality in patients with cirrhosis of different etiologies and severities of liver disease. The Model for End-Stage Liver Disease (MELD) is a scoring system for the severity of liver disease initially developed as a model in predicting poor survival in patients after transjugular intrahepatic porto-systemic shunt (TIPS). The lack of an assessment of renal function, which is a reliable prognostic marker in cirrhosis, is an additional limiting factor. The use of CTP in prioritizing potential liver transplant recipients is limited by several factors: the variables, ascites and encephalopathy, are all subjective and are influenced by medical therapy. The Child-Turcotte-Pugh (CTP) score, originally developed for the assessment of the outcome of patients with cirrhosis and portal hypertension, was extended for general prognosis, and to stratify patients on the waiting list for LTx. Liver transplantation (LTx) provides the only curative treatment option with excellent long-term results in patients with decompensated cirrhosis of the liver. This might have implications for the development of new improved scoring systems. The long term prediction of mortality or removal from waiting list in patients awaiting liver transplantation might be better assessed by the CTP score than the MELD score. This result was supported by the AUC analysis showing a strong trend for superiority of CTP over MELD scores (AUROC 0.73 and 0.68, resp. The sensitivity and specificity to identify mortality or severe deterioration for CTP was 69.0% and 70.5%, respectively for MELD, it was 62.1% and 72.7%, respectively. In the univariate analysis comparing patients who are still on the waiting list and patients who died or were removed from the waiting list due to poor conditions, the serum albumin, bilirubin INR, and CTP and MELD scores as well as the presence of ascites and encephalopathy were significantly different between the groups (p < 0.05), whereas serum creatinine and urea showed no difference.Ĭomparing the predictive abilities of CTP and MELD scores, the best discrimination between patients still alive on the waiting list and patients who died on or were removed from the waiting list was achieved at a CTP score of ≥9 and a MELD score of ≥14.4. The Mann-Whitney-U Test was used for the univariate analysis and the AUC-Model for discrimination of the scores. The predictive ability not only for mortality on the waiting list but also for the need for withdrawal from the waiting list was calculated for both scores. The Model for End-Stage Liver Disease (MELD) and Child-Turcotte-Pugh (CTP) scores of all patients at the time of listing were used for calculation. Methodsĭata sets of 268 consecutive patients listed for single-organ liver transplantation for nonfulminant liver disease between 20 were included into the study. The optimal strategy based on scoring systems and/or waiting time is still under debate. The relative shortage of organ donors renders the allocation algorithms of organs essential. Decompensated cirrhosis is associated with a poor prognosis and liver transplantation provides the only curative treatment option with excellent long-term results. 
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
